A Journey Home: How Oklahoma Children's OU Health Helped Ranger Beat the Odds

When Riggin and Mariah Dillis took their baby, Ranger, home for the first time on Jan. 12, 2026, the moment felt almost unreal. Their son had spent his entire life in the hospital since his birth more than nine months earlier. That homecoming marked the end of a long and complex medical journey and the beginning of a new chapter for their family.
Mariah sensed early in her pregnancy that something might not be right. Her mother had experienced preeclampsia, and Mariah herself had been born prematurely. Despite raising concerns with her doctor in Ardmore, her concerns weren’t fully addressed.
At 24 weeks pregnant, Mariah noticed swelling in her feet, ankles, face and hands. At her appointment, she was reassured everything was fine. But within days, she became so ill she could barely eat. When she returned for care the following week, her blood pressure was dangerously high.
“They told me my blood pressure was out of control, and they were going to have to care for me in Oklahoma City,” Mariah said.
A Tiny Beginning
 On April 11, 2025, at just 25 weeks’ gestation, Ranger Dillis was born weighing 1pound, 4 ounces and measuring 11 inches long.
On April 11, 2025, at just 25 weeks’ gestation, Ranger Dillis was born weighing 1pound, 4 ounces and measuring 11 inches long.
“He didn’t even fit in our hands,” Mariah said.
Because of his extreme prematurity, Ranger spent his first months at a local community hospital in Oklahoma City. Early in his care, doctors diagnosed him with bronchopulmonary dysplasia, a chronic lung condition that can affect babies born very early.
“They explained that the ventilator keeping him alive was also putting stress on his lungs,” Mariah said. “It was a double-edged sword.”
What Is Bronchopulmonary Dysplasia?
Bronchopulmonary dysplasia, often called BPD, is a chronic lung condition that most commonly affects babies born before 28 weeks of pregnancy. At that stage, the lungs are still developing. When premature infants need prolonged oxygen therapy or mechanical ventilation to survive, the fragile lung tissue can become inflamed or injured, disrupting normal growth.
Infants with BPD may require breathing support for months or longer. Oxygen needs can change from day to day, and many experience periods when breathing becomes more difficult before improvement begins. Lung health is closely tied to growth, nutrition, and brain development, which makes care especially demanding.
While many children with BPD improve as their lungs grow, progress is complex. Care requires long-term planning and close coordination across multiple specialties, with careful attention to both medical stability and development.
When Specialized Care Was Needed
Despite multiple attempts to reduce Ranger’s respiratory support, he could not maintain safe oxygen levels. His medical team recognized that he needed a level of care beyond what they could provide.
“They told us they maybe see a baby like Ranger once a year,” Mariah said.
Ranger was transported by medical jet to Dell Children’s in Austin, Texas. There, he received a tracheostomy and gastrostomy tube, both common interventions for infants with severe lung disease.
After about a month, doctors recommended another transfer, but this time closer to home.
“They said he needed to be closer to home to recover and eventually go home,” Mariah said. “So a jet took us from Austin to Oklahoma Children’s.”
Riggin was working in Oklahoma City, so the transfer also meant he could spend more time with his wife and son.
A Different Approach at Oklahoma Children’s
When Ranger arrived at Oklahoma Children's OU Health, part of the University of Oklahoma’s academic health system, he was critically ill. He was heavily sedated, medically paralyzed, and receiving medication doses that are uncommon in infants.
At Oklahoma Children’s, Ranger was cared for by pediatric critical care specialist Dr. Theresa Graif, M.D., an assistant professor of pediatrics at the University of Oklahoma College of Medicine, along with a specialized transitional care team. This team supports children with complex medical needs who no longer fit in a standard neonatal or pediatric intensive care unit.
“Children with severe BPD often experience a challenging period between 4 and 8 months of age, when lung disease can worsen before improvement begins,” Dr. Graif said. “Rather than rushing to reduce support, the team focused first on stabilizing Ranger, maintaining his comfort and protecting his development while his lungs healed.”
Care was deliberately paced. When an initial attempt to reduce sedation caused his carbon dioxide levels to rise too high, the team reassessed and adjusted the plan.
“They slowly weaned everything,” Mariah said. “It took months.”
Throughout that time, specialists across respiratory therapy, nutrition, rehabilitation, and Child Life worked together to support Ranger’s medical and developmental needs at the same time.
Parents as Part of the Care Team
A defining feature of Oklahoma Children’s transitional care model is the early and continuous involvement of families.
“Our program is designed so parents aren’t just trained at the end,” Dr. Graif said. “They’re involved throughout — even during unstable periods — so they truly know their child.”
Mariah stayed at the Ronald McDonald House on the OU Health Campus while Riggin, who works in the oil field in Oklahoma City, joined them each evening after work. Over time, they learned how to care for Ranger during both stable moments and more difficult ones.
After nearly four months, the family completed more than 40 hours of hands-on training, including simulation lab experiences, preparing them to care for Ranger at home with a tracheostomy and gastrostomy tube.
“It is absolutely phenomenal what they have going here,” Mariah said.
Going Home
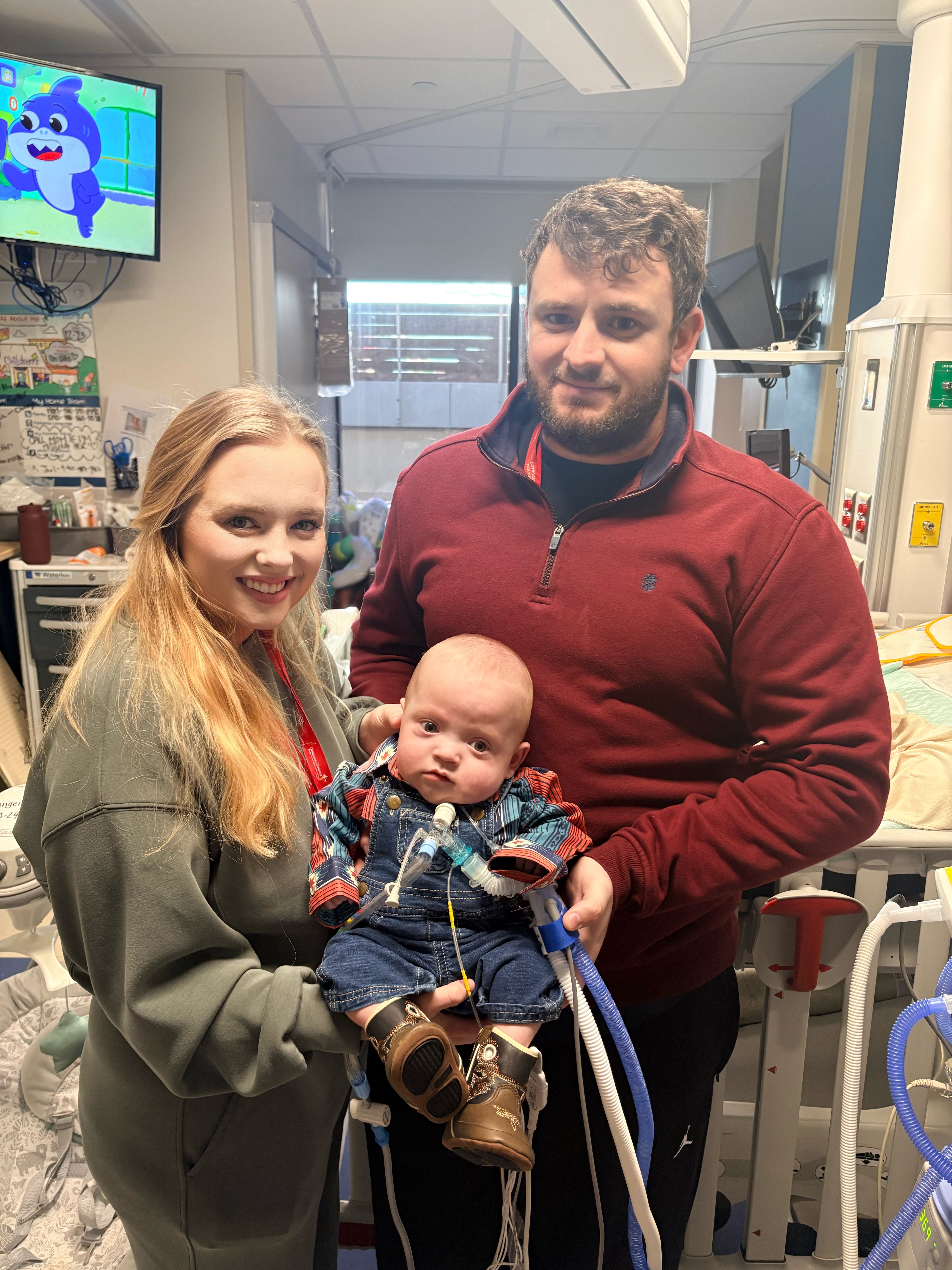 Now 9 months old (with an adjusted age of 6 months) Ranger continues to grow and develop. His lungs are healing with time, supported by his tracheostomy, which doctors expect he will need for the next few years.
Now 9 months old (with an adjusted age of 6 months) Ranger continues to grow and develop. His lungs are healing with time, supported by his tracheostomy, which doctors expect he will need for the next few years.
On discharge day, Oklahoma Children’s staff lined the halls to celebrate as Ranger headed home.
For a family whose journey spanned multiple cities and states, the care Ranger received at Oklahoma Children’s brought stability, continuity and a clear path forward.
“It’s a day-and-night difference since we arrived at Oklahoma Children’s and I would recommend them to anyone,” Mariah said.
When Oklahoma’s most complex cases need a way forward, Oklahoma Children’s doesn’t just provide care — we change what’s possible. Learn more about pulmonary and respiratory care services for children or speak with our team at (405) 271-2234.



